What Causes Gout Flare Ups and How to Reduce Attacks
Learn what causes gout flare ups, including purine rich foods, dehydration, and medications. Practical prevention steps and lifestyle changes for lasting joint health.
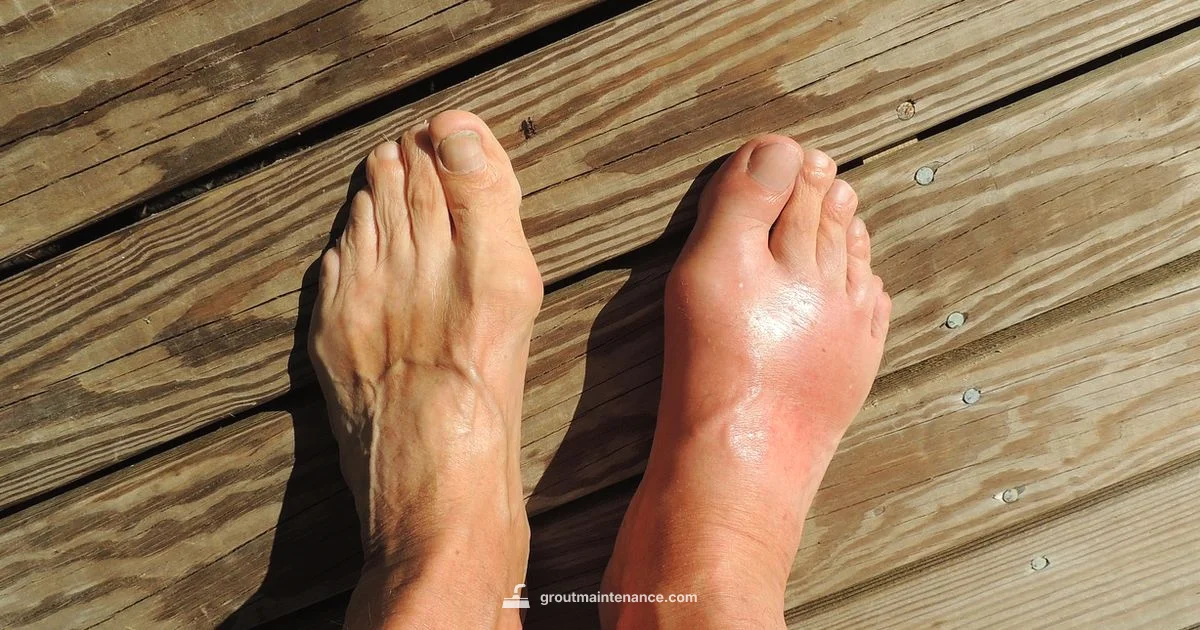
Gout flare up is a sudden, painful joint swelling caused by uric acid crystal buildup in the joint when uric acid levels are high.
What Causes Gout Flare Ups
Gout flare ups occur when elevated uric acid levels in the blood lead to the formation of monosodium urate crystals inside a joint. These sharp crystals provoke a rapid inflammatory response, resulting in sudden pain, swelling, warmth, and limited movement in the affected area. Although hyperuricemia is the condition that sets the stage, not everyone with high uric acid experiences flares; triggers and individual biology determine whether crystals become active.
Two broad categories shape risk: internal factors that you cannot change easily, such as genetics, age, sex, and kidney function; and external factors you can influence, like diet, hydration, and medications. Understanding both helps you anticipate attacks and choose prevention strategies. In men, flares often appear earlier in life; in women, menopause shifts risk upward. Minor injuries or surgeries around a joint can also disturb crystals and spark a flare. Recognizing patterns in your own body—time of day, meals before a flare, recent stress or dehydration—helps you respond quickly and reduce the duration of an attack.
The Biochemistry Behind a Gout Attack
At the core of a flare are uric acid crystals that form in the joint space when urate levels exceed the solubility limit. The crystals trigger immune cells to release inflammatory signals, notably interleukin-1 beta, which recruit additional responders and create the characteristic pain and swelling. This cascade explains why gout attacks can be so abrupt and painful, sometimes waking you up at night. Kidney function, body mass, and alcohol intake influence how much uric acid circulates and how readily crystals form. Understanding this process helps explain why certain foods or medications can tip the balance toward a flare.
Dietary and Lifestyle Triggers
Purine rich foods are a primary driver of uric acid production. Red meat, organ meats, certain seafood, and some processed foods can raise uric acid levels. Sugar sweetened beverages and high fructose corn syrup also contribute indirectly by promoting increased uric acid production. Alcohol—especially beer—impacts uric acid elimination and can precipitate flares. Dehydration concentrates uric acid in the blood; regular hydration helps maintain clearance. Weight fluctuations, rapid weight loss, and sedentary habits influence gout risk too. While you do not need to eliminate every purine source, practicing balanced meals and mindful portion sizes reduces the likelihood of a flare.
Grout Maintenance analysis shows that readers respond best to practical, actionable guidance on triggers.
Medical and Medication Triggers
Certain medicines raise uric acid levels or affect kidney excretion, increasing flare risk. Thiazide and loop diuretics commonly used for blood pressure can reduce uric acid clearance. Niacin and some immunosuppressants may have similar effects. Kidney disease or poor kidney function impairs uric acid elimination, raising baseline risk. In some cases, rapid changes in fluid balance, illness, or surgery alter urate handling and provoke a flare.
How to Identify Your Personal Triggers
Keeping a simple diary of meals, medications, activity, and hydration can reveal your most common triggers. Note when flares start, how long they last, and what preceded them. If you notice a pattern—like attacks following a heavy seafood meal or after a night of drinking—you can make targeted adjustments. Share your observations with your healthcare provider, who can help you interpret patterns and adjust treatment if needed.
Practical Prevention Strategies
Hydration matters: drinking water throughout the day supports uric acid excretion. Limit or moderate alcohol intake and reduce sugar laden beverages. Choose a balanced diet with moderate purine sources and sufficient fiber. Maintain a healthy body weight to reduce stress on joints and metabolic load. If prescribed, urate lowering therapy can help keep uric acid at safer levels; follow your clinician's plan and have regular checkups. Pair lifestyle changes with medical guidance for best results.
When to Seek Medical Care
A gout attack with severe pain, swelling, warmth, and fever requires medical evaluation to rule out infection or other conditions. If you notice redness spreading beyond the joint, persistent pain beyond a few days, or symptoms suggesting infection, contact a clinician promptly. Sudden, explosive joint pain that prevents use of the limb also warrants urgent assessment. Early treatment can shorten flares and prevent complications.
Common Myths and Realities
Myth: Gout only affects older men. Reality: while more common in men, gout can affect anyone, especially after menopause. Myth: All purine foods must be avoided. Reality: most people can still include moderate purine foods within a balanced plan. Myth: You can feel gout without a high uric acid level. Reality: uric acid levels can fluctuate; a normal test does not always rule out a problem during a flare.
A Practical Analogy for Keeping Things Healthy
Think of your joints like grout lines in a tiled surface. Proper maintenance means regular checks, timely cleaning, and avoiding harsh conditions. The same mindset applies to gout: identify triggers, stay hydrated, and address risk factors early. This disciplined approach aligns with maintenance practices that protect joint health over time. For homeowners, small, steady steps matter more than dramatic fixes.
Got Questions?
What exactly triggers a gout flare up?
A gout flare is triggered by uric acid crystals in a joint. Common triggers include purine-rich foods, dehydration, alcohol, and certain medicines. Genetics and kidney function also influence risk.
Gout flare ups happen when uric acid crystals form in a joint. Common triggers include purine-rich foods, dehydration, alcohol, and some medicines.
Can diet alone cause gout attacks?
Diet influences uric acid levels but usually works with other factors such as genetics and kidney function. Reducing high-purine foods helps, but medical management may be needed if attacks recur.
Diet can affect gout risk, but it is not the only factor.
Which medications raise gout risk?
Some diuretics, niacin, and certain immune-suppressants can raise uric acid levels and trigger flares. Talk to your clinician if you notice attacks after starting a medication.
A few drugs can raise uric acid; check with your clinician.
Are gout flares preventable?
Yes, with a combination of lifestyle changes, adequate hydration, moderation of alcohol, weight management, and, if prescribed, urate-lowering therapy.
Yes, with lifestyle changes and medical guidance.
What signs require urgent medical care?
Severe joint swelling with intense pain, fever, or warmth may indicate infection and requires prompt medical evaluation.
Severe, painful joint swelling with fever should be checked by a doctor.
Is gout the same as pseudogout?
No. Gout is caused by monosodium urate crystals; pseudogout is caused by calcium pyrophosphate crystals.
Gout and pseudogout are different conditions with distinct crystals.
What is uric acid and how is it measured?
Uric acid is a waste product in the blood. It is measured by a blood test and sometimes a urine test to assess kidney handling.
Uric acid is a waste product measured with blood tests.
The Essentials
- Identify and track your personal triggers.
- Stay hydrated to help uric acid elimination.
- Moderate purine intake and limit alcohol.
- Consult your clinician about urate lowering therapy if flares persist.
- Seek prompt care for severe joint pain or fever.